|
|
Frostbite
General Considerations
- Injury to tissue due to freezing and crystallization of intra- and extracellular fluids from cold
- Risk factors include diabetics, African-Americans, previous history of frostbite and certain medications, like beta-blockers
- Mostly occurs on hands, feet, nose, ears and lips
- High-altitude frostbite combines hypoxia, dehydration and tissue freezing and has a worse prognosis
Clinical Findings
- Coldness, stinging or burning
- Numbness and/or complete loss of sensation
- Loss of fine muscle movements
- Severe joint pain
- Hyperemia, blue discoloration, skin necrosis, gangrene
Imaging Findings
- The diagnosis is made on a clinical basis
- Conventional radiography may show
- Atrophy of the distal tuft
- Acro-osteolysis of distal phalanx/phalanges
- Soft-tissue swelling
- Radioscintography using Technetium-99m may help in identifying non-viable soft tissue
- MRI may also be helpful in assessing tissue viability
Differential Diagnosis
- Acro-osteolysis from another cause, e.g., hyperparathyroidism, congenital insensitivity to pain, leprosy, scleroderma
Treatment
- Rapidly re-warm body part
- Hydration
- Ibuprofen
Prognosis
- Healing can take 6-12 months
- Absence of edema, hemorrhagic blebs, persistent cyanosis and anesthesia after rewarming are poor prognostic indicators
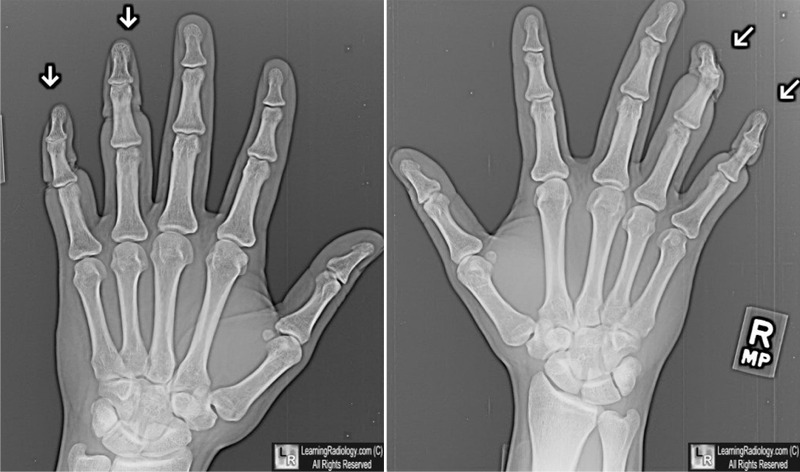
Frostbite. Soft-tissue technique for both hands shows chronic changes of soft tissue loss of the terminal phalanges of both ring and little fingers (white arrows). The patient had sustained frostbite injuries to these fingers 4 weeks earlier.
Frostbite. CC Mechem, D Cheng, R Yakobi, TM Thompson. eMedicine.
The Soft-Tissue and Bone Changes in Frostbite Injuries. Jack M. Tishler. Radiology, March 1972, Vol. 102, Issue 3.
|
|
|