|
|
Pericardial Calcifications
Constrictive Pericarditis
- Calcification in the pericardium is most likely
inflammatory in nature
- Can be seen with a variety of infections,
trauma, and neoplasms
- Calcification most commonly occurs along the
inferior diaphragmatic surface of the pericardium surrounding the
ventricles
- Thin, egg-shell like calcification is more often
associated with viral infection or uremia
- Calcification from old TB is often thick,
confluent, and irregular in appearance, especially when compared with
myocardial calcification
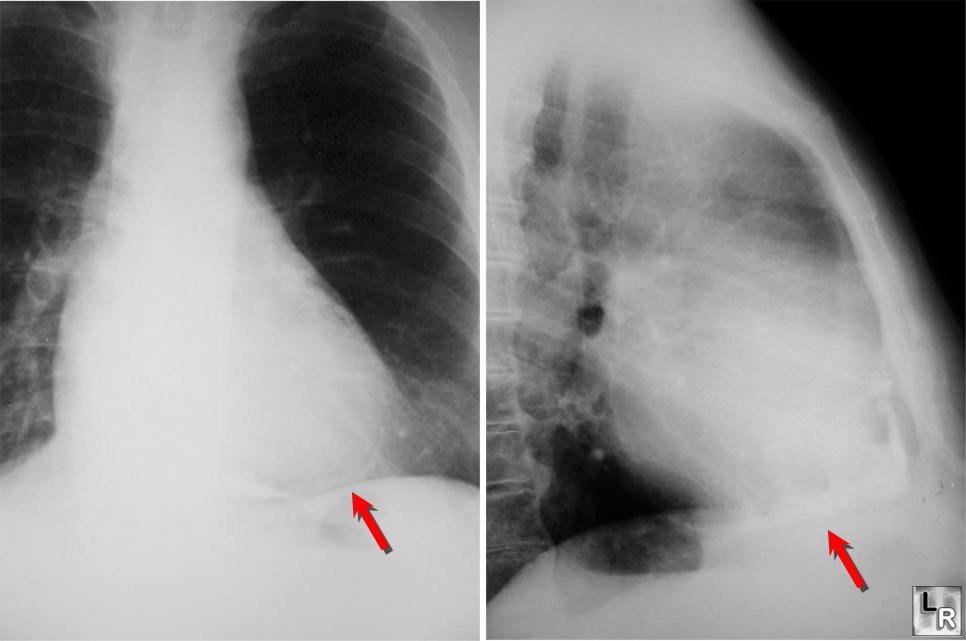
PA and
lateral close-ups show thick pericardial calcification around
apex of heart from patient with history of tuberculous pericarditis
- Calcification is seen in 1/3-1/2 of patients with
constrictive pericarditis
- Its presence does not imply constriction
- Pericardial calcification must be differentiated
from coronary artery calcification, valvular calcification, calcified
myocardial infarct or ventricular aneurysm, left atrial calcification,
or calcification outside the heart
- This can usually be accomplished by the
locations of these calcifications on multiple views, or the
radiographic appearance of the calcium
- Constrictive Pericarditis
- Present when a fibrotic, thickened, and adherent
pericardium restricts diastolic filling of the heart.
- Usually begins with an initial episode of acute
pericarditis
- May not be detected clinically
- This slowly progresses to a chronic stage
consisting of fibrous scarring and thickening of the pericardium with
obliteration of the pericardial space
- This produces uniform restriction of the filling
of all heart chambers
- Signs and Symptoms
- Reduced cardiac output ( fatigue, hypotension,
reflex tachycardia )
- Elevated systemic venous pressure ( jugular
venous distension, hepatomegaly with marked ascites and peripheral
edema )
- Pulmonary venous congestion ( exertional
dyspnea, cough and orthopnea )
- Chest pain typical of angina may be related to underperfusion of the coronary arteries or
compression of an epicardial coronary
artery by the thickened pericardium.
- Most impressive physical findings are often the
insidious development of ascites of hepatomegaly and ascites, such
patients are often mistakenly thought to suffer from hepatic cirrhosis
or an intra-abdominal tumor.
· Calcification of
the pericardium is detected in up to 50 % of patients
· This finding is
not specific for constrictive pericarditis
o A calcified
pericardium is not necessarily a constricted one
o Lateral chest
film is useful for its detection in the atrioventricular groove or along
the anterior and diaphragmatic surfaces of the right ventricle.
o Pleural effusions
are present in about 60 % of patients
§ Persistent
unexplained pleural effusions can be the presenting manifestation
· CT or MRI are
superior in the assessment of pericardial anatomy and thickness
· The diagnosis is
confirmed by cardiac catheterization
· Treatment for
constrictive pericarditis is complete resection of the pericardium
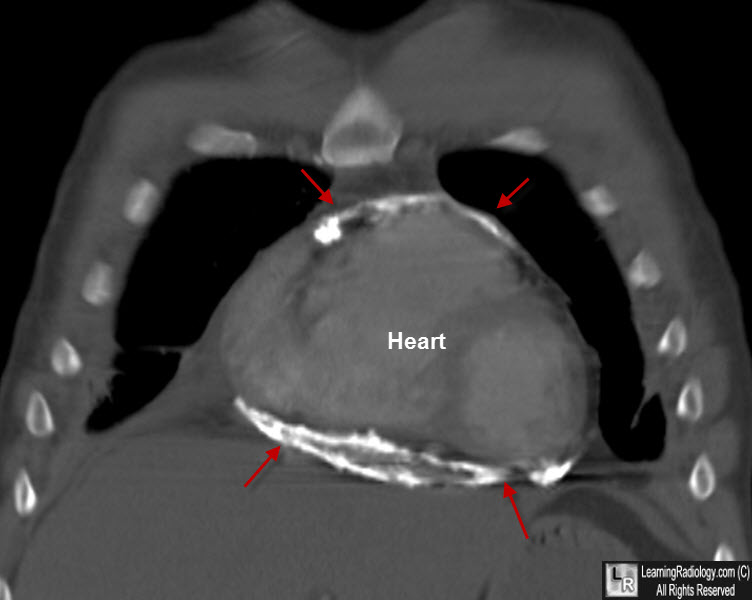
Constrictive Pericarditis. Coronal re-formatted CT of chest shows markedly thick pericardial calcification around
the heart from patient with history of tuberculous pericarditis.
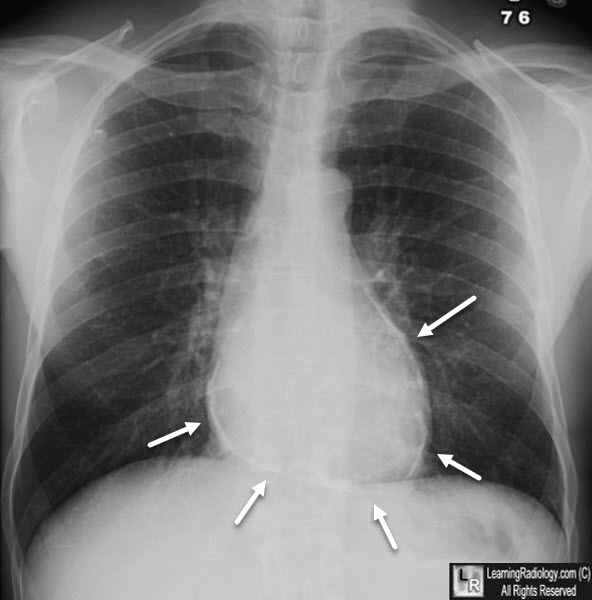
Constrictive Pericarditis. Frontal chest radiograph shows curvilinear calcification surrounding the heart consistent with calcific pericarditis.
Acknowledgement to Eduardo Benchimol Saad, MD
|
|
|